Obstructive Cardiomyopathy: A Comprehensive Overview
Hypertrophic Obstructive Cardiomyopathy (HOCM) is a subtype of hypertrophic cardiomyopathy characterized by abnormal thickening of the myocardium, predominantly affecting the interventricular septum. This hypertrophy can impede blood flow from the left ventricle into the aorta, posing significant hemodynamic challenges. HOCM is a relatively rare disorder, with a prevalence of approximately 1 in 500 individuals, yet its implications for cardiovascular health are profound. Understanding the condition requires a multidisciplinary approach, encompassing insights from genetics, imaging, and interventional cardiology to ensure accurate diagnosis and effective management.
 |
| Image source Google |
Pathophysiology
The pathophysiological hallmark of obstructive cardiomyopathy is asymmetric septal hypertrophy, which narrows the left ventricular outflow tract (LVOT) and disrupts normal hemodynamics. The resultant obstruction generates increased intraventricular pressure, which can provoke systolic anterior motion (SAM) of the mitral valve leaflets, further contributing to LVOT obstruction and mitral regurgitation. As the hypertrophied myocardium becomes less compliant, diastolic dysfunction ensues, leading to impaired ventricular filling. Over time, chronic pressure overload may result in myocardial fibrosis, which increases the risk of arrhythmias and sudden cardiac death. Genetic mutations, particularly in sarcomeric proteins such as beta-myosin heavy chain (MYH7) and myosin-binding protein C (MYBPC3), underpin most cases of HOCM, leading to aberrant myocardial structure and function.
Etiology and Risk Factors
HOCM is primarily an autosomal dominant genetic disorder, with variable penetrance and expression. Key risk factors include:
- Genetic Predisposition: Mutations in genes encoding sarcomeric proteins are the most common cause.
- Age: Symptoms typically manifest in adolescence or early adulthood but may present later in life.
- Sex: Males may present with more pronounced hypertrophy, though the condition affects both sexes.
- Exercise: High-intensity activities can exacerbate symptoms and increase the risk of sudden cardiac events.
- Family History: First-degree relatives of affected individuals have a 50% chance of inheriting the genetic mutation.
- Other Factors: Obesity, hypertension, and metabolic syndrome can further contribute to disease progression.
Clinical Manifestations
The clinical presentation of HOCM is diverse, ranging from asymptomatic cases to severe heart failure. Common symptoms include:
- Exertional Dyspnea: Difficulty breathing during physical activity due to increased LVOT obstruction.
- Angina Pectoris: Chest pain resulting from myocardial oxygen demand exceeding supply.
- Syncope: Transient loss of consciousness, often precipitated by exertion or arrhythmias.
- Palpitations and Arrhythmias: Sensation of irregular heartbeats due to underlying electrical disturbances.
- Fatigue and Reduced Exercise Tolerance: Secondary to impaired cardiac output and diastolic dysfunction. In some cases, patients may remain asymptomatic, and the condition is only detected during routine screening or family evaluations.
Diagnostic Evaluation
A thorough diagnostic workup is crucial for identifying HOCM and assessing disease severity:
- Physical Examination: Detection of a harsh systolic murmur, often accentuated with Valsalva maneuver, is suggestive of LVOT obstruction.
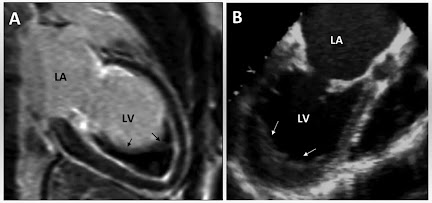
- Echocardiography: Gold standard for visualizing septal hypertrophy, LVOT obstruction, and mitral valve anomalies. Doppler studies provide insights into pressure gradients across the outflow tract.
- Electrocardiography (ECG): May reveal left ventricular hypertrophy, Q waves, or arrhythmias.
- Cardiac MRI/CT: Provides detailed myocardial characterization, assessment of fibrosis, and delineation of myocardial architecture.
- Genetic Testing: Identifies pathogenic mutations, aiding in family screening and risk stratification.
- Exercise Stress Testing: Evaluates exertional symptoms and the presence of inducible LVOT obstruction.
- Holter Monitoring: Assesses for paroxysmal arrhythmias, particularly in patients with palpitations or syncope.
Complications
Without proper management, HOCM can lead to severe complications, such as:
- Sudden Cardiac Death: Particularly in young athletes, due to lethal arrhythmias.
- Progressive Heart Failure: Resulting from diastolic dysfunction and elevated filling pressures.
- Life-Threatening Arrhythmias: Including ventricular tachycardia and fibrillation.
- Mitral Valve Dysfunction: Contributing to further hemodynamic instability and exacerbation of symptoms.
- Infective Endocarditis: Rare but possible, due to turbulent blood flow across abnormal structures.
Therapeutic Approaches
Management strategies for HOCM aim to alleviate symptoms and reduce the risk of sudden cardiac death:
- Pharmacologic Therapy: Beta-blockers and calcium channel blockers mitigate symptoms by reducing myocardial contractility and heart rate. Disopyramide may be used to reduce obstruction.
- Invasive Interventions:
- Septal Myectomy: Surgical removal of hypertrophic septal tissue to relieve LVOT obstruction.
- Alcohol Septal Ablation: Induces localized myocardial infarction to reduce septal thickness.
- Implantable Cardioverter-Defibrillator (ICD): Prevents sudden cardiac death in high-risk patients.
- Lifestyle Modifications: Restriction from competitive sports and strenuous activities. Avoiding dehydration and maintaining electrolyte balance are also crucial.
Long-Term Management and Prognosis
Long-term care involves periodic monitoring of cardiac function and symptom progression. Risk stratification for sudden cardiac death is crucial and involves assessing factors like family history, extent of hypertrophy, and prior arrhythmic events. The prognosis is highly variable, influenced by genetic factors, the degree of hypertrophy, and adherence to treatment regimens. Many patients can achieve a normal lifespan with appropriate medical and surgical management, though some may require heart transplantation in refractory cases.
Preventative Measures
Preventing adverse outcomes in HOCM requires a multifaceted approach:
- Regular cardiovascular screening for first-degree relatives.
- Genetic counseling for at-risk families.
- Adoption of heart-healthy behaviors, such as maintaining optimal blood pressure, avoiding excessive physical exertion, and adhering to prescribed therapies.
- Awareness programs aimed at recognizing warning signs early, especially in athletic populations.
Coping with HOCM
Living with HOCM demands not only physical adaptation but also emotional resilience. Accessing psychosocial support, engaging with patient advocacy groups, and staying informed about emerging therapies can empower individuals to navigate their condition more effectively. Patients should be encouraged to maintain an active dialogue with their healthcare providers and participate in shared decision-making regarding treatment options.
Conclusion
Obstructive cardiomyopathy is a complex genetic disorder with profound implications for cardiovascular health. Advances in diagnostic modalities and therapeutic interventions have greatly improved patient outcomes. Early diagnosis, tailored treatment strategies, and ongoing research remain pivotal in enhancing the quality of life for affected individuals. As understanding of the condition continues to evolve, future therapies hold promise for even better management and prognosis.
References
- Maron, B. J., Ommen, S. R., Semsarian, C., Spirito, P., Olivotto, I., & Maron, M. S. (2014). Hypertrophic cardiomyopathy: present and future, with translation into contemporary cardiovascular medicine. Journal of the American College of Cardiology, 64(1), 83-99.
- Elliott, P. M., Anastasakis, A., Borger, M. A., Borggrefe, M., Cecchi, F., Charron, P., ... & Watkins, H. (2014). 2014 ESC Guidelines on diagnosis and management of hypertrophic cardiomyopathy. European Heart Journal, 35(39), 2733-2779.
- Ho, C. Y., & Seidman, C. E. (2006). A contemporary approach to hypertrophic cardiomyopathy. Circulation, 113(24), e858-e862.




No comments:
Post a Comment
Please do not enter any spam link in the comment box